After a Few Setbacks, My Port Has Made Infusions Much Easier
Written by |

Just over a year ago, I started a new biologic. As part of my preparation to begin this treatment, I needed to have a power port placed in my chest because I would be having infusions every two weeks.
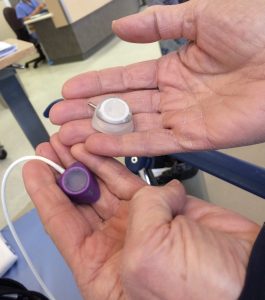
A power port is a small, round medical device with a catheter attached. This device is surgically implanted under the skin in the chest, and then the catheter is inserted into one of the central veins that carries blood to the heart.
The port is used as an access point for infusions, but can also be used for blood draws or contrast dyes used for medical imaging in place of an IV.
A few months before I started my new biologic, I had the opportunity to talk to other rare disease patients who were on the same treatment about their ports and how they worked. It helped reassure me about the entire process of getting and using one, and I was grateful for their insight.
Since I was the first patient my neurologist had ever put on this brand new biologic, they weren’t aware that a port was necessary. But once I explained what I’d learned from other patients, they understood and sent a referral to an interventional radiologist to book what would be an outpatient surgery.
On the morning of my surgery, the nurse brought two examples of the ports they use to show me what they look like. They gave me medicine through my IV to help me relax before injecting the surgical area with a local anesthetic. While I couldn’t see what was going on because of the way I was draped, I was awake and could hear everything.
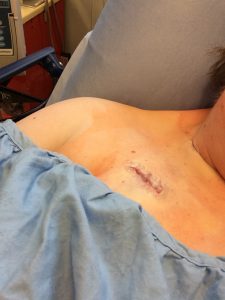
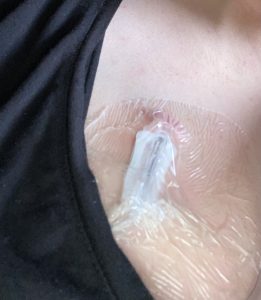
The surgery took about 45 minutes. The two relatively small incisions were closed with dissolvable stitches and steri-strips that I could remove after a few days. I spent about an hour in recovery before going home.
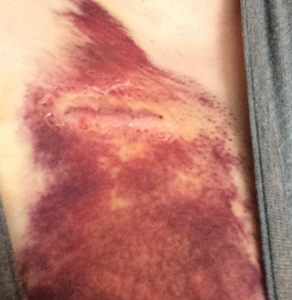
Sleeping for the first few nights was challenging because my chest was sore — not from the incisions, but from the epic (and I mean epic!) bruising from the implant. Moving the tissue to make room to tuck the port in securely created a wicked black and purple bruise the size of a football.
Trying to find a comfortable position to lie in was nearly impossible. That deep, ugly bruise took weeks to fade.
The first time a nurse tried to access the port for an iron infusion, it was an absolute failure. They use three different sizes of needles, and despite trying all three, she was unsuccessful. This made me quite anxious because I was about to start my new biologic, and it seemed there may have been a problem with my port.
(Spoiler alert: There wasn’t a problem with my port. I later learned that the failure was due to bad technique.)
When I finally started my biologic, I bought an over-the-counter topical analgesic cream and put it on the skin where my port was located. I anticipated being poked a number of times because of my unfortunate first experience, and I definitely didn’t want to feel it. Luckily, the nurse that was taking care of me was much more skilled at accessing ports and had no trouble getting in on the first try. That was a huge relief.
The downside of having a port is that just 10 months after I’d received it, it suddenly stopped working. My infusion nurse, who comes to infuse me at home, thought I may have developed a blood clot somewhere in the catheter.
I immediately called the interventional radiologist, who saw me the next day. He put some contrast dye through my port and could see exactly what the problem was: A small piece of tissue had grown over the end of the catheter. It was acting like a flap; they could push fluid into the vein, but when they went to draw fluid out (called “getting return”), the suction caused the tissue to move, slamming the line shut.
I had to laugh when he told me that this is extremely rare, and he’d never seen it happen with the kind of port I have. If it’s rare, it will happen to me. I had to have another surgery to remove the tissue. My port has — touch wood — worked perfectly ever since.
The upside of having a port is the easy access. No more digging for veins or bruised hands, since it can be used in place of an IV. As long as my port is used once a month, it’s fine. When not in use, it has to be flushed monthly with heparin to keep it in working order. Having my port accessed is painless compared to having IVs and has made my infusions so much easier.
***
Note: Neuromyelitis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Neuromyelitis News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to neuromyelitis optica spectrum disorder.





Leave a comment
Fill in the required fields to post. Your email address will not be published.